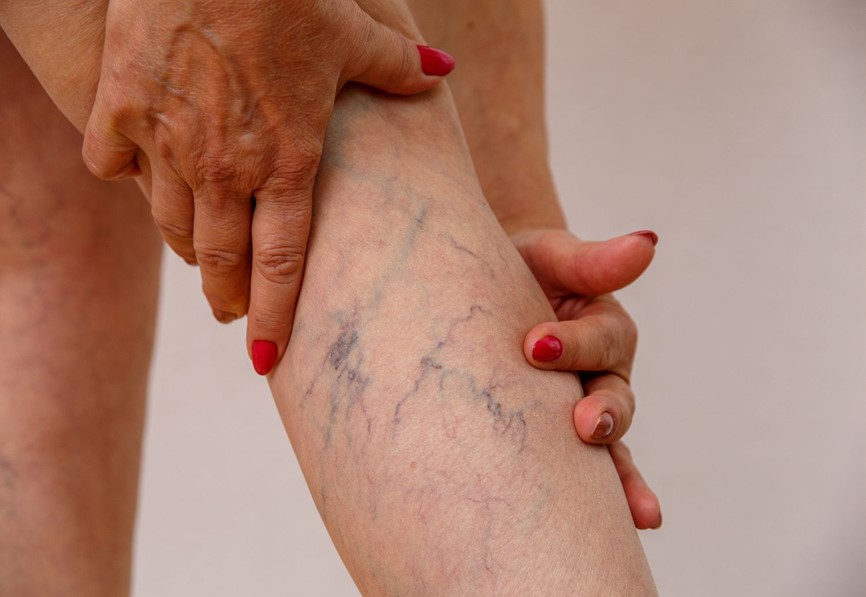
21 Oct Understanding Varicose Veins – Symptoms, Causes, Risk Factors And Treatment
Welcome to an exploration of varicose veins and spider veins, common conditions affecting the veins in our legs. Varicose veins may appear when blood flow encounters difficulty, causing veins to swell and become noticeable under the skin.
Standing for long periods can add pressure to the veins, potentially leading to the development of varicose veins. These veins can also be linked to deep vein thrombosis, a concerning issue within the deep veins. Recognizing the symptoms of varicose veins is vital; from aching legs to visible veins, understanding these signs is crucial for timely treatment.
Fortunately, treatments are available to address varicose veins and alleviate discomfort, offering relief to those affected by this condition. Stay tuned to discover more about the causes, symptoms, and treatment options for varicose veins and spider veins.
Understanding Symptoms of Varicose Veins
Varicose veins are a common type of swollen and twisted veins, primarily found in the legs. These veins have weakened walls that can’t pump blood as effectively, causing the blood to pool and the veins to bulge. Here are some common symptoms associated with varicose veins:
1. Visible Swelling and Bulging Veins: Varicose veins often appear as enlarged, twisted veins under the skin, giving a swollen and rope-like appearance. They are usually found in the legs.
2. Aching and Discomfort: People with varicose veins may experience aching, throbbing, or a sense of heaviness in their legs. This discomfort can worsen after standing or sitting for extended periods.
3. Itching and Skin Changes: The skin around varicose veins may become itchy or irritated. Over time, the skin near the affected veins might darken or develop a leathery texture.
4. Muscle Cramping and Restlessness: Some individuals may experience muscle cramping or a restless feeling in their legs, especially at night. This can disrupt sleep and daily activities.
5. Pain and Tenderness: Varicose veins can cause localized pain and tenderness, especially when touched or pressed. This discomfort can range from mild to severe, particularly in cases of severe varicose veins.
6. Fatigue and Weakness: Individuals with varicose veins might notice increased fatigue and weakness in their legs, especially towards the end of the day or after prolonged periods of standing or walking.
7. Complications and Ulcers: Severe varicose veins may lead to complications such as skin ulcers, where the skin near the veins breaks down and forms open sores. This can be painful and may require medical attention.
It’s important to remember that varicose veins can be influenced by several factors, including family history, prolonged standing or sitting, and the presence of other risk factors. Seeking timely medical advice and following recommended procedures can help manage symptoms of varicose veins from getting worse.
How Are Varicose Veins Diagnosed?
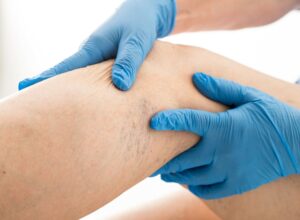
Here’s how medical professionals diagnose varicose veins:
1. Physical Examination: When you suspect you may have varicose veins, your doctor will start with a physical examination. They will visually inspect your legs, looking for bulging veins, swelling, and skin discoloration. They may also ask about any symptoms you’re experiencing, like pain or heaviness in the legs.
2. Medical History: Your doctor will take a detailed medical history, including any family history of varicose veins or other related conditions. Understanding your health background helps in determining risk factors and potential causes of varicose veins.
3. Ultrasound Examination: To get a clear picture of the veins beneath the skin’s surface, an ultrasound examination is often conducted. This non-invasive test uses sound waves to create an image of the veins in your legs, allowing the doctor to assess the blood flow and detect any abnormalities.
4. Doppler Test: Doppler ultrasound is a specialized type of ultrasound that evaluates the blood flow in the veins. It helps identify if the valves in the veins are functioning properly and if there is any reflux (backward flow of blood) contributing to varicose veins.
5. Venography: In some cases, a venography may be performed. This involves injecting a contrast dye into a large vein in your foot or ankle. X-rays are then taken to trace the dye’s movement, giving a detailed view of the veins and any blockages or abnormalities.
6. CT or MRI Scan: Computed tomography (CT) or magnetic resonance imaging (MRI) scans may be used to create detailed images of the veins. These advanced imaging techniques can help evaluate the extent and type of varicose veins.
7. Consultation with a Vascular Specialist: Depending on the complexity of the varicose veins, your doctor may refer you to a vascular specialist, such as a vascular surgeon or a phlebologist. These specialists have expertise in diagnosing and treating various types of varicose veins, providing tailored treatment recommendations.
What Causes Varicose Veins?
Understanding what causes varicose veins can help in managing and alleviating the discomfort they bring.
Increased Pressure in the Veins:
Varicose veins are caused by increased pressure in the veins, especially in the veins near the surface of the skin. This elevated pressure makes the veins become enlarged and appear as varicose veins. The veins in our legs have one-way valves that help blood flow towards the heart. When these valves weaken or become damaged, blood can flow backward and accumulate, causing varicose veins.
Weakening of Vein Structure:
The structure of the veins can weaken over time, making them less efficient in pushing blood back to the heart. This weakening can be due to various factors such as age, obesity, or prolonged standing or sitting, which may add more pressure on the veins and prevent proper blood circulation.
Heredity and Genetic Predisposition:
Varicose veins can also be inherited. If your family members have a history of varicose veins, you may be more susceptible to developing them too. Genetic factors can influence the strength and structure of your veins, making you prone to varicosities.
Pregnancy and Hormonal Changes:
Hormonal changes during pregnancy can affect the veins, making them more susceptible to enlargement. The increased pressure on the veins in your pelvic area due to the growing uterus can cause varicose veins to develop during pregnancy. Hormonal fluctuations can weaken vein walls, exacerbating the condition
Lack of Physical Activity and Diet:
A sedentary lifestyle and a diet lacking in fiber can contribute to varicose veins. Regular exercise helps in maintaining healthy blood circulation and prevents the buildup of pressure in the veins. A diet rich in fiber supports good digestion and overall cardiovascular health, indirectly influencing vein health.
Occupational Factors:
Certain occupations that involve prolonged periods of standing or sitting can increase the risk of varicose veins. Professions that demand long hours on your feet or in a seated position can hinder proper blood flow, leading to the development of varicosities.
Diagnostic and Treatment Procedures:
If you experience discomfort from varicose veins, seeking medical advice is crucial. Diagnostic procedures for varicose veins may include ultrasound imaging to assess the condition of the veins and determine the best course of action. Treatments to remove varicose veins may include minimally invasive procedures like endovenous laser treatment or sclerotherapy, which can help improve blood flow and alleviate symptoms.
Maintaining a healthy lifestyle, staying physically active, and seeking appropriate medical care can help in minimizing the impact of varicose veins on daily life.
Treatment for Varicose Veins
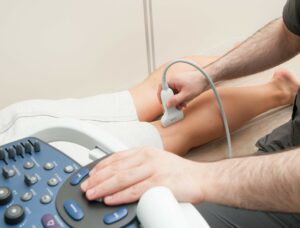
People who have varicose veins may experience discomfort, pain, and aching in their legs. In severe cases, these symptoms may even lead to skin ulcers.
Recognizing the Signs of Varicose Veins
If you suspect you have varicose veins or notice any of the signs mentioned, it’s essential to seek treatment. Varicose veins can happen to anyone, but certain factors, such as genetics, pregnancy, and prolonged standing, can increase the risk of developing them. It’s important to remember that varicose veins are not just a cosmetic issue; they can impact your overall health and well-being. Therefore, if you experience any of the symptoms, it’s time to consider treatment.
Non-Invasive Approaches to Manage Varicose Veins
Thankfully, there are various treatment options available to manage varicose veins. These treatments can help improve the appearance of your veins, relieve discomfort, and prevent complications. Here are some non-invasive approaches to consider:
1. Lifestyle Modifications: Making certain lifestyle changes can be the first step in managing varicose veins. Regular exercise, maintaining a healthy weight, and elevating your legs when resting can help reduce symptoms.
2. Compression Stockings: These are special stockings that provide external pressure to the veins, helping to improve blood flow and alleviate discomfort.
3. Sclerotherapy: A common treatment for smaller varicose veins and spider veins, this procedure involves injecting a solution into the affected veins, causing them to collapse and fade.
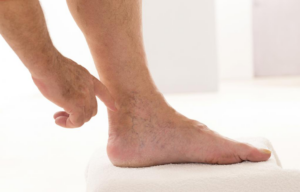
Spider Vein Treatment In Nanuet Ny
Minimally Invasive and Surgical Options
For more severe cases, or when conservative treatments do not yield desired results, minimally invasive or surgical procedures may be recommended. These include:
4. Endovenous Laser Ablation (EVLA): A minimally invasive procedure that uses laser energy to close off the problematic vein.
5. Radiofrequency Ablation (RFA): Similar to EVLA but using radiofrequency energy to heat and seal the affected vein.
6. Ambulatory Phlebectomy: A surgical procedure that involves physically removing the varicose veins through tiny incisions.
Consulting a Healthcare Professional
If you suspect that you have varicose veins, it’s essential to consult a healthcare professional who specializes in vein disorders. They can assess your condition, discuss your symptoms, and recommend the most appropriate treatment plan for you. While varicose veins may also be a cosmetic concern, addressing the underlying issues is vital to prevent complications and make your varicose veins a thing of the past.
How To Prevent Varicose Veins Naturally
Here are some natural tips to help you keep varicose veins at bay:
1. Maintain a Healthy Weight: Being overweight can increase the pressure on your veins, making it more likely for varicose veins to develop. To prevent this, try to maintain a healthy weight through a balanced diet and regular exercise. This can help to prevent blood from pooling in your leg veins.
2. Stay Active: Regular physical activity is a key factor in preventing varicose veins. Exercise helps to improve blood circulation, preventing the blood from stagnating in your veins. Simple activities like walking, swimming, or cycling can make a significant difference.
3. Elevate Your Legs: If you have a job that requires long periods of sitting or standing, make an effort to elevate your legs when you can. This will help reduce pressure inside your veins and prevent blood from pooling, which can lead to varicose veins.
4. Wear Compression Stockings: Compression stockings are designed to apply gentle pressure to your legs, helping your veins to work more efficiently. These can be particularly useful for individuals at an increased risk of developing varicose veins or those who have already experienced them.
5. Eat a Balanced Diet: A diet rich in fiber, fruits, and vegetables can promote healthy veins. Foods high in fiber help prevent constipation, which can increase pressure on your veins. Additionally, vitamin C and antioxidants in fruits and vegetables support blood vessel health.
6. Stay Hydrated: Proper hydration is crucial for maintaining healthy veins. Drinking enough water ensures that your blood remains thin and flows smoothly through your vessels. Dehydration can make varicose veins worse, so be sure to drink plenty of water throughout the day.
7. Avoid High Heels and Tight Clothing: High-heeled shoes can disrupt the natural pumping action of your calf muscles, which squeeze the deep veins to propel blood upwards. Also, avoid tight clothing that can restrict blood flow in your groin and waist area.
In cases where varicose veins are already present, medical treatments may be necessary. Procedures like radiofrequency energy or injections into the varicose veins can be used to treat varicose veins. These therapies, often done by a doctor, can help alleviate the symptoms and improve the appearance of the affected area.
Risk Factors For Varicose Veins
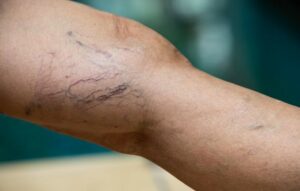
Knowing these risk factors and symptoms can help in managing and preventing this common condition.
1. Genetic Predisposition: Varicose veins are often hereditary. If someone in your family has experienced varicose veins, you may be more susceptible. The weakening of the vein walls can be inherited, making the occurrence of varicose veins more likely.
2. Age and Vein Health: As we age, the veins in our legs may naturally weaken, affecting the efficiency of the one-way valves. This can cause blood to pool in the veins, resulting in the enlargement of varicose veins.
3. Hormonal Influence and Gender: Women are more prone to varicose veins due to hormonal changes, such as those during pregnancy or while using birth control. These hormonal shifts can weaken vein walls and valves, increasing the risk of varicose veins.
4. Lifestyle Choices: Long periods of standing or sitting can elevate pressure in the veins, potentially causing veins to weaken and become varicose. Regular physical activity can help in maintaining healthy blood circulation.
5. Obesity and Excessive Pressure: Being overweight or obese can exert excess pressure on leg veins. This added pressure weakens the veins and contributes to the developing of varicose veins.
6. Trauma and Blood Clots: Injuries to the legs or blood clots can damage the veins, leading to the varicose veins. Medical interventions, such as injecting medication or using radiofrequency energy via a catheter, can aid in treating varicose veins effectively.
Conclusion
In summary, understanding varicose veins is essential for making informed decisions about treatment. Medical procedures like radiofrequency energy being inserted into the varicose veins through a catheter offer effective solutions. This method can help manage the discomfort and appearance of varicose veins, promoting better circulation and overall leg health.
By exploring these modern treatments, individuals can take proactive steps toward alleviating the challenges posed by varicose veins and improving their quality of life. Always consult a healthcare professional to determine the best approach for your specific situation
Frequently Asked Questions
What are varicose veins, and how do they occur?
Varicose veins are enlarged, swollen veins that occur when the walls of the superficial veins in the legs weaken, causing the veins to become enlarged. This happens because the veins have one-way valves that help blood flow towards the heart. When these valves malfunction or weaken, blood can pool in the veins and damage the valves, resulting in varicose veins.
What are the common symptoms of varicose veins?
Common symptoms of varicose veins include visible, twisted, and bulging veins near the surface of the skin, often in the legs. Other symptoms include aching, heaviness, or discomfort in the legs, and sometimes varicose veins can cause the affected areas to itch or burn. It’s essential to consult a healthcare professional if you experience these symptoms.
Are varicose veins a common condition?
Yes, varicose veins are a common condition, especially among adults. They can affect both men and women, although women are more often affected. The prevalence increases with age and other factors such as pregnancy, obesity, and a sedentary lifestyle. Understanding the causes and seeking appropriate medical advice can help manage varicose veins effectively.
What are the potential complications of varicose veins?
If left untreated, varicose veins can lead to complications such as chronic venous insufficiency, skin changes or ulcers, and superficial thrombophlebitis (inflammation of the veins). Additionally, varicose veins can be a source of discomfort and negatively impact one’s quality of life. Seeking early intervention and discussing treatment options with a healthcare provider is important to prevent complications.
How are varicose veins treated?
Varicose veins can be treated through various methods. Non-invasive treatments include lifestyle changes like exercise and elevating the legs, using compression stockings, and sclerotherapy, where a solution is injected into the varicose veins to close them. In more severe cases, procedures like endovenous laser treatment or vein stripping, where a catheter or a thin tube is inserted into a varicose vein, might be recommended. The appropriate treatment will depend on the severity and individual circumstances, so it’s best to consult a healthcare professional.
Can varicose veins occur in other parts of the body aside from the legs?
Varicose veins usually develop in the veins of the legs. The walls of the veins weaken, causing the veins to become swollen and twisted. These enlarged veins are commonly known as varicose veins. In some cases, similar enlarged veins, often smaller and closer to the skin’s surface, may also appear on the face, particularly around the nose and cheeks, known as spider veins.
Are varicose veins considered a serious medical condition?
Varicose veins are not considered a life-threatening condition. However, they can cause discomfort and affect one’s quality of life. The pressure in your veins due to weakened walls and malfunctioning one-way valves can lead to the development of new varicose veins. While not life-threatening, seeking medical advice for proper evaluation and management is important to alleviate symptoms and prevent potential complications.
Can anything be done to strengthen the walls of veins and help blood flow?
While the walls of the veins weaken in varicose veins, certain lifestyle changes and medical interventions can help manage the condition. Regular exercise, maintaining a healthy weight, and elevating the legs can assist in improving blood circulation and reducing the pressure in your veins. Compression stockings can also support the veins and aid in blood flow. Medical treatments such as sclerotherapy and endovenous laser treatment may be recommended to treat existing varicose veins and potentially strengthen the affected veins. Always consult a healthcare professional for personalized advice.
Read more:
Understanding Varicose Veins: Diagnosis and Treatment Options

goltogel
Posted at 09:59h, 12 JanuaryInformative read, I recommend it!
udintogel
Posted at 10:58h, 12 JanuaryThis article is amazing! The way it clarifies things is absolutely captivating and extremely easy to follow. It’s clear that a lot of work and investigation went into this, which is indeed commendable. The author has managed to make the subject not only interesting but also delightful to read. I’m wholeheartedly excited about exploring more information like this in the forthcoming. Thanks for sharing, you’re doing an amazing work!
Mixzaimus
Posted at 14:11h, 12 JanuaryСломался мой старый холодильник, и семейные ужины стали настоящей проблемой. Но благодаря социальным сетям, я узнал о сайте msk-zaim.ru, где был представлен список новых МФО 2024 года. Подав заявку, я был поражен скорости одобрения и перевода денег на мою банковскую карту. Теперь моя семья может наслаждаться вкусными ужинами, благодаря новому холодильнику.
Займы онлайн – на ремонт кондиционера
Mixzaimus
Posted at 16:48h, 12 JanuaryСтиральная машина сломалась, и моя жизнь стала намного менее комфортной. Я начал искать способы замены её, но бюджет был ограничен. В одной из групп в социальной сети я наткнулся на рекламу сайта, где представлен огромный список новых МФО 2024 года. С помощью этого сайта, мне удалось получить займ моментально и купить новую стиральную машину. Теперь моя бытовая жизнь стала намного удобнее.
Займы срочно – возьмите займ на покупку ноутбука